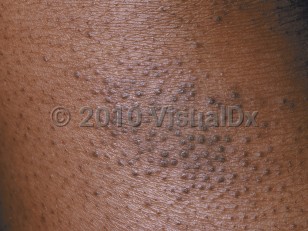
In infants, the disease involves primarily the face, scalp, and torso. In children and adults, the disease usually involves chiefly the flexural aspects of extremities, but it may be more generalized.
Atopic dermatitis may be categorized as follows:
- Acute – erythema, vesicles, bullae, weeping, crusting
- Subacute – scaly plaques, papules, round erosions, crusts
- Chronic eczema – lichenification, scaling, hyper- and hypopigmentation
The cause of atopic dermatitis is unknown. Genetic and environmental predisposing factors exist. Multiple loci have been associated with atopic dermatitis. A family history of atopic dermatitis is common.
Intense pruritus (itching) is a hallmark of atopic dermatitis. Scratching leads to lichenification (skin thickening from chronic trauma). Eyelid skin may be involved with scaly or lichenified plaques. Impaired barrier function leads to increased transepidermal water loss and the risk of bacterial and viral cutaneous infections. Patients with atopic dermatitis are prone to impetiginization with Staphylococcus aureus (impetigo). Secondary infections with herpes simplex virus (eczema herpeticum), molluscum contagiosum, Coxsackie virus, or vaccinia virus (eczema vaccinatum) can occur.
Patients with atopic dermatitis have difficulties in retaining skin moisture and suffer from xerosis (dry skin). Environmental triggers, such as heat, humidity, detergents / soaps, abrasive clothing, chemicals, smoke, and even stress, tend to aggravate the condition. Latex allergy and nickel allergy occur more often in persons with atopic dermatitis. Additionally, patients with atopic dermatitis have been found to be more likely to have positive patch test results to products commonly found in topical treatments, including cocamidopropyl betaine, wool alcohol / lanolin, and tixocortol pivalate. Allergy to eggs, cow's milk, or peanuts is common. There may be a relationship between atopic dermatitis and the development of aspirin-related respiratory disease.
Atopic keratoconjunctivitis is characterized by ocular pruritus, burning, and tearing. It is usually associated with concomitant dermatitis and asthma and affects 20%-40% of those with dermatitis, being seen somewhat more often in males.
Posterior subcapsular cataracts are typically asymptomatic and can be seen in adult patients with severe atopy. They rarely occur in children. Factors driving the development of cataracts in atopic dermatitis may be the disease itself or corticosteroid therapy. Keratoconus is reported in about 1% of patients with atopic dermatitis and appears to develop independently of cataract formation.



 Patient Information for
Patient Information for