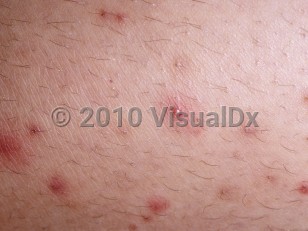
Folliculitis in Adult
See also in: Anogenital,Hair and ScalpAlerts and Notices
Important News & Links
Synopsis

The etiology of folliculitis can be variable, with bacterial, fungal, viral, parasitic, and noninfectious causes reported. A detailed history of comorbid conditions, exposures, and medications, in conjunction with appropriate ancillary testing, can be helpful.
In immunocompetent patients, bacterial folliculitis may be considered, often due to a predisposing factor that allows for increased bacterial burden on the skin surface. Staphylococcus aureus and Streptococcus species are commonly implicated. Predisposing factors include nasal carriage of S. aureus, occlusion, maceration, hyperhydration, complicating pruritic skin diseases, vigorous application of topical medications, shaving (folliculitis barbae / sycosis barbae), exposure to oils and certain chemicals, and exposure to heated or contaminated water.
For example, a history of contaminated water exposure was suspected in an outbreak of folliculitis due to atypical mycobacteria in otherwise healthy adults who had recently undergone pedicures. Folliculitis due to Pseudomonas aeruginosa has similarly been linked to contaminated water exposure from swimming pools.
These predisposing factors have also been associated with infectious folliculitis due to nonbacterial causes. A history of shaving or other hair-removal procedures has been associated with folliculitis due to molluscum contagiosum and dermatophyte infection (tinea barbae), as well as noninfectious folliculitis due to a foreign body reaction (pseudofolliculitis barbae).
Fungal causes of folliculitis in immunocompetent hosts additionally include Pityrosporum (Malassezia) spp. and dermatophyte infection of the hair follicle (including fungal folliculitis and Majocchi granuloma). Pustular folliculitis secondary to Candida spp. (see candidiasis) has also been reported in immunocompetent adults, particularly in skin folds.
Viral folliculitis secondary to varicella zoster virus (usually a primary phenomenon), herpes simplex virus (usually inoculated secondary to shaving), and molluscum contagiosum have been described.
In immunocompromised patients, folliculitis can occur secondary to etiologies similar to those discussed above. For example, bacterial folliculitis may evolve into furunculosis, or inflammation involving deeper aspects of the pilosebaceous unit, in patients with certain risk factors such as diabetes mellitus, immunosuppression, or human immunodeficiency virus (HIV) infection. Fungal folliculitis secondary to Candida albicans has been reported in immunocompromised patients, particularly in the setting of candidemia.
In addition to these etiologies, more esoteric causes must also be kept in mind when considering the immunocompromised host. For example, Demodex spp. are mites that infest the follicles and sebaceous glands of normal adults, but have been associated with a pruritic perifollicular papulopustular eruption on the face of immunocompetent adults or with a more widespread eruption in immunocompromised adults and children. Eosinophilic pustular folliculitis presenting as pruritic urticarial follicular papules is seen in immunocompetent hosts (the Ofuji variant) or in hosts immunosuppressed by HIV infection or hematologic disorders (immunosuppression-associated eosinophilic folliculitis). During pregnancy, a pruritic folliculitis has been reported with no associated morbidity to the fetus or mother and that clears spontaneously after delivery.
A careful medication history is required. Exposure to prolonged periods of antibiotic therapy results in disruption of the normal gram-positive skin flora and is a risk factor for the development of gram-negative folliculitis. Other medications associated with follicular eruptions include corticosteroids, epidermal growth factor receptor inhibitors, sirolimus, cyclosporine, lithium, lamotrigine, aripiprazole, chlorpromazine, dantrolene, dapsone, and halogens (potassium iodide, radiocontrast media).
Codes
L73.8 – Other specified follicular disorders
SNOMEDCT:
13600006 – Folliculitis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
Drug Reaction Data
Subscription Required
References
Subscription Required
Last Updated:03/22/2023
 Patient Information for Folliculitis in Adult
Patient Information for Folliculitis in Adult- Improve treatment compliance
- Reduce after-hours questions
- Increase patient engagement and satisfaction
- Written in clear, easy-to-understand language. No confusing jargon.
- Available in English and Spanish
- Print out or email directly to your patient