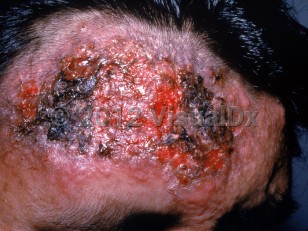
Botryomycosis - Cellulitis DDx
See also in: OverviewSynopsis

Two-thirds of patients have skin involvement. Lesions develop slowly over weeks and months. These patients usually have no systemic symptoms, although local pain and pruritus may occur. A visceral form (usually involving the lungs but sometimes disseminating to the kidneys, liver, or nodes) may rarely occur. Visceral forms may be primary or may occur as a result of cutaneous extension.
Approximately 40% of cases of botryomycosis are due to Staphylococcus aureus, with Pseudomonas spp. causing another 20% of cases. Other reported causative bacteria include Proteus, Moraxella, Serratia, Escherichia coli, Corynebacteria, and streptococci.
Disease is reported worldwide. A history of local injury is common. Patients with low T-cell counts are predisposed to developing botryomycosis, as are patients with alcoholic liver disease, diabetes, human immunodeficiency virus (HIV), cystic fibrosis, hyper-IgE syndrome, and those on chronic corticosteroids. It rarely occurs in healthy individuals. The pathogenesis most likely represents an interaction between bacterial load, the organism's virulence, and the host's immunity.
Botryomycosis may be confused with cellulitis. Immunosuppression and the finding of lesions discharging a granular, purulent drainage should prompt consideration of this diagnosis.
Codes
B48.8 – Other specified mycoses
SNOMEDCT:
238413001 – Botryomycosis
Look For
Subscription Required
Diagnostic Pearls
Subscription Required
Differential Diagnosis & Pitfalls

Subscription Required
Best Tests
Subscription Required
Management Pearls
Subscription Required
Therapy
Subscription Required
References
Subscription Required
Last Updated:01/07/2019